For years, Type 2 Diabetes has been viewed through two dominant lenses: blood sugar and heart disease. But a third threat has been growing in silence.
It is not dramatic.
It is not usually painful.
And in many patients, it remains completely undetected.
That threat is liver fibrosis—the slow, silent scarring of the liver that may already be developing in a substantial proportion of people living with Type 2 Diabetes.
The New Evidence India Can No Longer Ignore
A major multicentre Indian study published in The Lancet Regional Health – Southeast Asia has delivered a serious warning. Among 9,202 asymptomatic adults with Type 2 Diabetes:
- 65% had hepatic steatosis.
- 26% had clinically significant liver fibrosis.
- 14% had advanced fibrosis.
- 5% had probable cirrhosis.
These were not patients coming to liver clinics with obvious symptoms. They were adults with diabetes who largely felt well. That is the real danger. In Type 2 Diabetes, serious liver disease may already be present before the patient feels anything at all. The liver can continue to accumulate fat, inflammation, and scar tissue quietly—long before it forces itself into the clinical conversation.
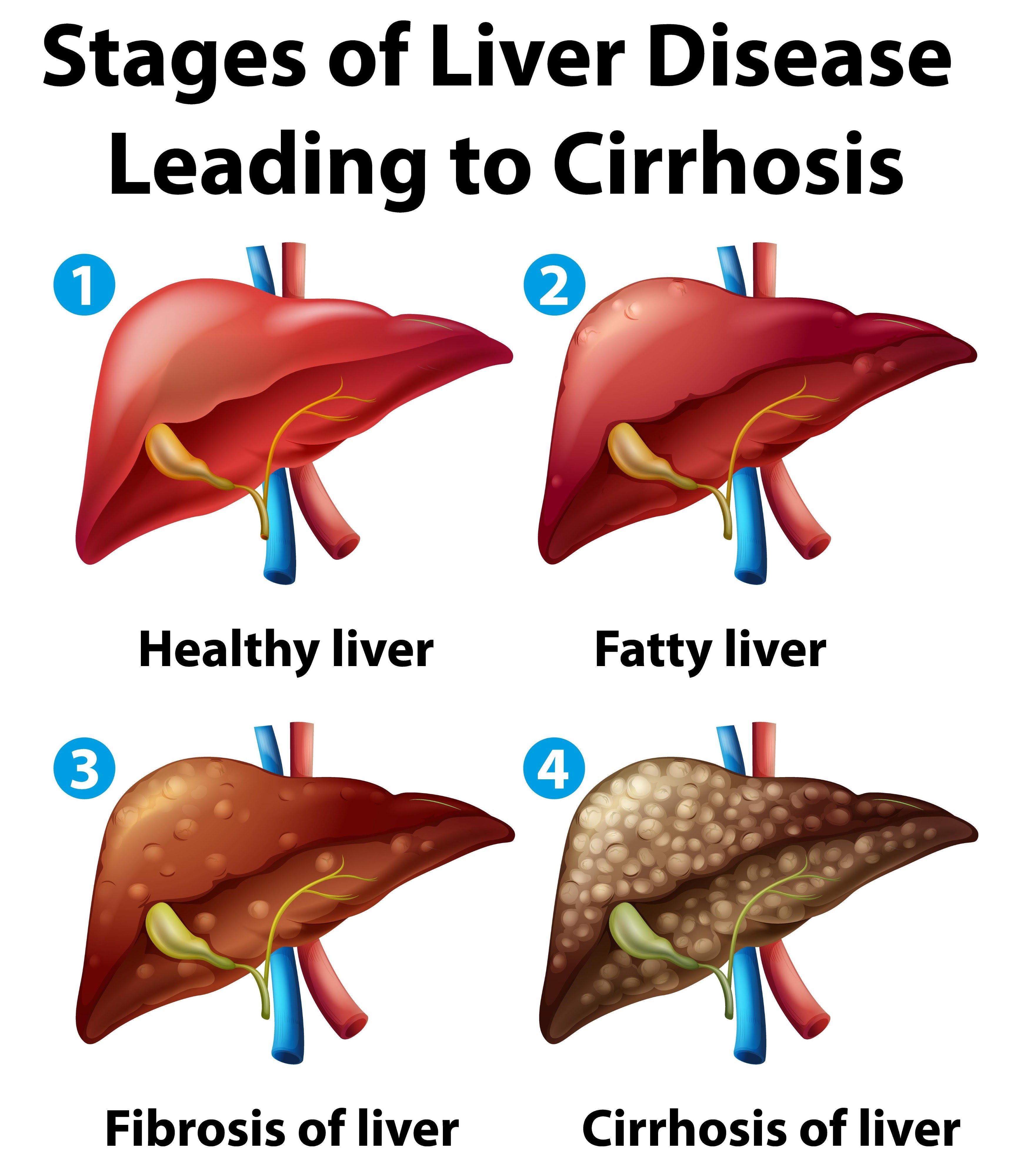
What Is Actually Happening Inside the Liver?
The process usually begins with excess fat building up inside liver cells. Today, this condition is called MASLD—Metabolic Dysfunction-Associated Steatotic Liver Disease.
- MASLD: Simple fatty buildup.
- MASH: Fat progresses to inflammation and cellular injury.
- Fibrosis: Healthy liver tissue is gradually replaced by scar tissue.
Once fibrosis advances, the stakes rise sharply: cirrhosis, liver failure, portal hypertension, liver cancer, and transplant risk all become part of the future trajectory.
Why Type 2 Diabetes Accelerates Liver Damage
This is not an accidental overlap. It is a biological partnership. Type 2 Diabetes creates exactly the conditions that drive liver injury forward:
- Insulin resistance
- Excess liver fat
- Chronic inflammation
- Oxidative stress
- Metabolic overload
Diabetes should not be seen as only a glucose disorder. It is a multi-organ metabolic disease, and the liver is one of its most vulnerable targets. An Indian multicentre biopsy-based study found that Type 2 Diabetes was associated with nearly double the odds of advanced fibrosis in patients with MASLD.
The South Asian Paradox
This issue may be even more dangerous in Indian and South Asian populations. Many patients do not look conventionally “obese.” They may appear only mildly overweight—or even normal by BMI—yet still carry:
- High visceral fat
- Marked insulin resistance
- Central obesity
This is the exact metabolic pattern that drives both premature cardiovascular disease and fatty liver progression. In other words, the heart story and the liver story are not separate stories. They are two expressions of the same metabolic dysfunction.
The Most Dangerous Feature: Silence
Heart disease often gets attention because it can announce itself with pain. Liver fibrosis usually does not.
- No chest pressure.
- No dramatic early warning.
- No obvious day-to-day disability.
That is why so many patients remain undiagnosed until the disease is already well established. The absence of symptoms does not mean the absence of damage. In fact, the DiaFib-Liver study specifically examined adults who were asymptomatic for liver disease.
A National Problem, Not a Niche Problem
This is not a rare complication confined to specialist centres. Indian data showed meaningful regional variation in fibrosis prevalence:
- 21% in Central India.
- 30% in Southern India.
This is a reminder that the burden is broad, national, and shaped by a mix of lifestyle, metabolic risk, and regional patterns of disease. This is no longer a side issue in diabetes care; it is part of the core disease burden.
Screening: The Missing Link in Diabetes Care
Patients with Type 2 Diabetes should not wait for liver symptoms before being evaluated. Current expert guidance recommends a two-tier pathway:
- First Tier: A simple blood-based score such as FIB-4.
- Second Tier: If indicated, a non-invasive test such as transient elastography (FibroScan/VCTE) or the ELF test.
Fibrosis can often be identified before symptoms begin, when intervention still has the greatest chance to change the future.
Treatment: A New Era Has Begun
The landscape has shifted from purely lifestyle-based management to a new era of therapeutics:
- March 2024: FDA approved resmetirom (Rezdiffra) for adults with noncirrhotic MASH with moderate to advanced fibrosis.
- August 2025: FDA approved semaglutide (Wegovy) for MASH with moderate-to-advanced fibrosis. (In phase 3 studies, 63% achieved MASH resolution).
- Emerging: Survodutide outperformed placebo in phase 2 trials for MASH improvement without worsening fibrosis.
The story is no longer just one of hidden disease; it is now also a story of earlier detection and real therapeutic opportunity.
Why This Matters Beyond the Liver
MASLD is increasingly linked with a higher risk of:
- Coronary artery disease & Myocardial infarction
- Stroke
- Atrial fibrillation
- Heart failure
A higher FIB-4 index is associated with increased all-cause and cardiovascular mortality. Liver fibrosis is not just a liver metric—it is a broader risk signal.
What Should Change—Starting Now
For Patients
Do not assume that a normal day-to-day feeling means your liver is safe. Ask your doctor about assessment for fatty liver and fibrosis—especially if you have abdominal obesity, elevated triglycerides, or long-standing diabetes.
For Clinicians
Liver risk should be built into routine diabetes care—not treated as an optional add-on. Non-invasive fibrosis tools are now practical, scalable, and essential.
For Health Systems and Policy Makers
This is a public health blind spot. Diabetes strategies that ignore liver fibrosis are no longer complete. Screening pathways and awareness campaigns are urgently needed.
The Final Truth
The next major complication of diabetes is not “coming soon.” It is already here.
- It is silent.
- It is progressive.
- It is still undiagnosed.
We once focused only on sugar. Then we learned to fear the heart. Now it is time to recognise the liver. Because by the time the liver finally speaks, the disease may already be far advanced.
Prevention is no longer optional. It is strategy.
Medical Disclaimer
This content is for educational purposes only and is not a substitute for professional medical advice. Individuals with existing medical conditions or high cardiovascular risk should consult their healthcare provider before starting any new exercise routine.
ARTICLE AUTHOR
Dr. Kamales Kumar Saha
Clinician–Leader · Cardiac Surgeon· Preventive Cardiologist · IICA-Certified Independent Director, Author : The Silent Epidemic
Dr. Kamales Kumar Saha is a seasoned Clinician–Leader with boardroom judgment, combining deep expertise in cardiac surgery and preventive cardiology with strategic healthcare leadership. His work bridges clinical excellence and patient education— helping patients make informed, sustainable health decisions.
Copyright Notice
© 2026 Dr Kamales Kumar Saha. All rights reserved.
No part of this blog may be reproduced, stored in a retrieval system, or transmitted in any form or by any means: electronic, mechanical, photocopying, recording, or otherwise without the prior written permission of the author, except for brief quotations used in reviews or scholarly references. This book is intended for personal reading only and may not be redistributed, resold, or reproduced in any format without permission.